
-
Orbital inflammatory disease
The spectrum of orbital inflammatory disease ranges broadly from specific disease diagnoses to nonspecific inflammation. Orbital inflammatory disease may be secondary to an underlying systemic inflammatory disease or may represent localized pathologic processes without systemic involvement.
-
Specific orbital inflammatory disease
Systemic inflammatory diseases associations of orbital inflammation include sarcoidosis, Wegener’s granulomatosis, Crohn’s disease, systemic lupus erythematosis, Churg–Strauss, Erdheim–Chester, histiocytosis X, etc.
The sclerosing variant of orbital inflammation is uncommon, but produces serious morbidity with a severe, chronic, progressive syndrome often characterized by proptosis, mild external inflammatory signs, restricted motility, diplopia, and dull, chronic pain. Diagnosis is typically made by orbital biopsy in which there is evidence for scarring and fibrosis. Sclerosing orbital inflammation shares some features with and may be related to systemic fibrosclerotic diseases involving the retroperitoneum.
IgG4-related disease (IgG4-RD) is a relatively recently recognized fibroinflammatory condition of unknown etiology characterized by elevated serum IgG4, but nearly 50% of biopsy proven and clinically active systemic IgG4-RD may have normal serum IgG4 levels.
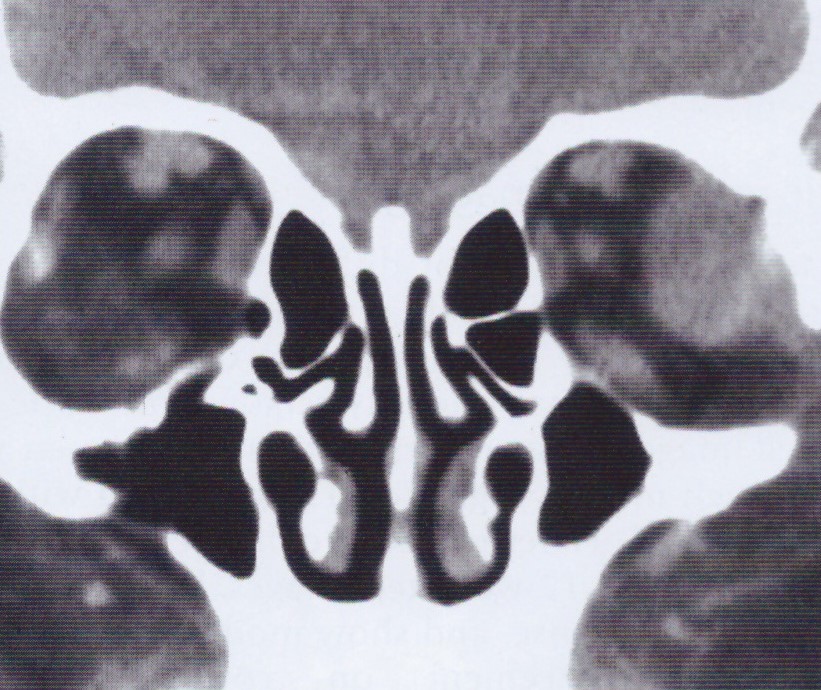
-
Idiopathic orbital inflammatory disease
Idiopathic orbital inflammatory disease, also known as nonspecific orbital inflammation, or orbital pseudotumour (term which is best to be avoided) is, by definition, a diagnosis of exclusion and neoplastic, infectious, and systemic inflammatory or immunologic causes must be excluded.
Any orbital tissue can be involved and presentation varies from acute to chronic. Idiopathic orbital inflammatory disease can be localized or diffuse.
When localized, inflammation can affect the extraocular muscles (orbital myositis), the lacrimal gland (dacryoadenitis), the optic nerve sheath (perineuritis), the sclera, episclera, Tenon's capsule, and uvea. It may also affect the orbital apex or present as a focal mass. When diffuse, idiopathic orbital inflammatory disease may diffusely involve the orbital fatty tissues.
-
Symptoms of idiopathic orbital inflammatory disease
Clinical symptoms consist of abrupt pain, swelling, erythema, proptosis, and restriction of eye movements. The clinical course varies, and spontaneous regression may occur in a few patients.
In severe cases, mass effects can cause secondary optic nerve atrophy, disc edema, and complete visual loss.
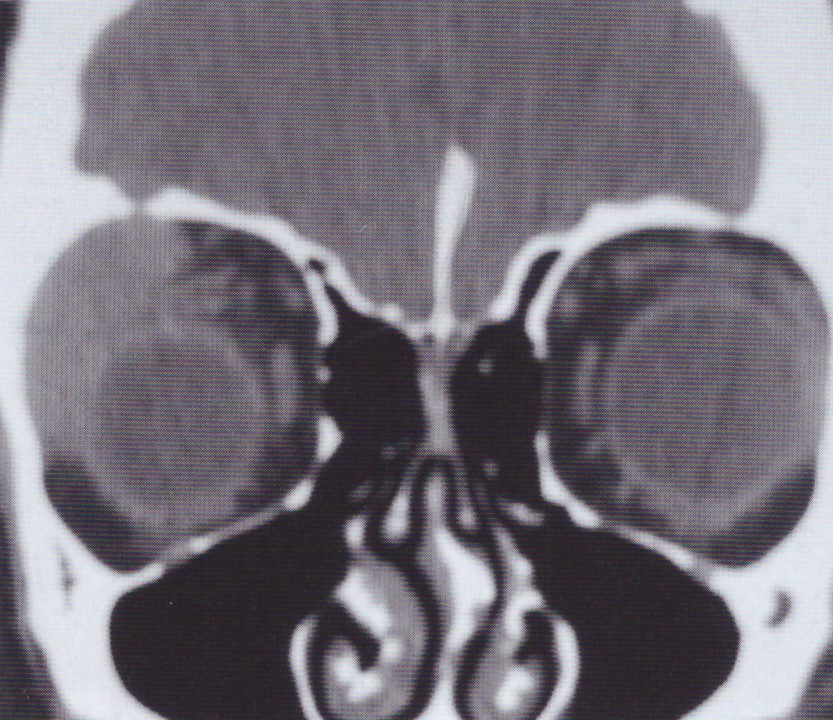
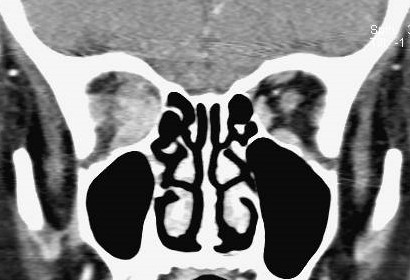
-
Evaluation of the patient with suspected idiopathic orbital inflammatory disease
Evaluation of the patient with suspected idiopathic orbital inflammatory disease must include a careful history, physical examination, directed laboratory, and radiologic studies, frequently involving high-resolution computed tomography (CT) or contrast-enhanced magnetic resonance imaging (MRI), and may require tissue biopsy for diagnostic studies.
-
Differential diagnosis of idiopathic orbital inflammatory disease
There are many processes that can mimic idiopathic orbital inflammatory disease. The most common orbital processes that present with similar clinical pictures are thyroid eye disease and orbital cellulitis.
-
Management of idiopathic orbital inflammatory disease
High-dose corticosteroids, the adult daily dose typically in the range of 60–80 mg of prednisone, is the mainstay initial therapy for acute or subacute idiopathic orbital inflammatory disease.
Typically, response to corticosteroids is rapid with a dramatic improvement in all symptoms and findings, but steroid taper must be performed slowly over period of weeks to months in order to prevent exacerbation or recurrence of inflammation.
Long term steroid therapy is complicated by adverse events including mood or weight changes, hyperglycaemia, dyspepsia, or accelerated bone changes in patients who are at risk for osteoporosis.
Corticosteroids alter both the clinical course and histopathologic findings in idiopathic orbital inflammatory disease.
Therefore corticosteroids should be used only after a tissue diagnosis is established, with the following exceptions:
- Superior orbital fissure syndrome
- Classic orbital myositis
- Classic thyroid eye disease
- Sight-threatening orbital inflammatory disease awaiting urgent biopsy
Although corticosteroids are typically used in initial therapy, some chronic forms of idiopathic orbital inflammatory disease may be poorly responsive and require other therapeutic modalities including radiation therapy or immunomodulators such as Methotrexate, Cyclosporine-A, Azathioprine, Cyclophosphamide, Adalimumab, Infliximab, Rituximab, Tocilizumab etc.
Eyelid, Lacrimal & Orbital Diseases
Learn more about the disease you are interested in

